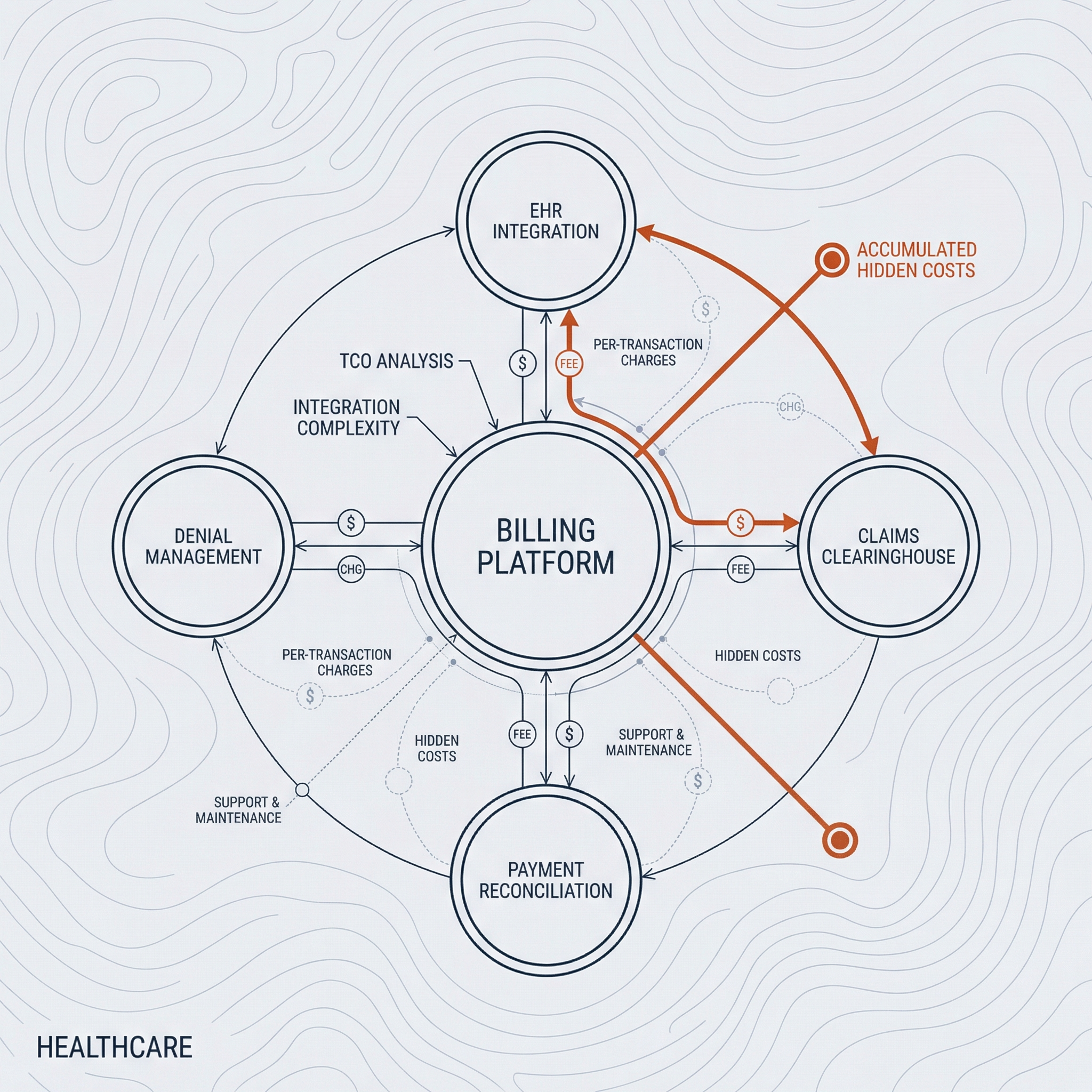
Investing in medical billing software promises streamlined workflows and optimized revenue cycle management. Yet, many practices discover that the sticker price rarely matches the true cost. Hidden fees, implementation challenges and ongoing maintenance expenses can erode margins and complicate budgeting. This article examines the drivers behind these unexpected expenditures and presents actionable strategies to mitigate them, empowering healthcare leaders to maintain financial predictability without sacrificing operational efficiency.
The True Cost of Medical Billing Software
Medical billing software sits at the center of the modern revenue cycle, but the initial purchase price often represents just a fraction of total expenses. Beyond licensing fees, practices may face implementation charges, training costs, integration fees and per-claim surcharges. According to a recent analysis in Medical Economics, these additional line items can increase overall spending by 20–30%, turning what seemed like a cost-saving solution into a budgetary burden.
Software vendors sometimes bundle modules or lock key features behind higher-tier packages, requiring upgrades to handle denials management, reporting or multi-payer connectivity. Without a granular breakdown of costs, healthcare administrators risk underestimating their financial commitment and facing unwelcome surprises in subsequent budget cycles.
Key Drivers of Hidden Costs
Understanding the root causes of unanticipated expenses is critical for crafting a robust procurement strategy. The primary drivers include:
1. Integration Complexity: Combining billing platforms with electronic health records (EHRs), practice management systems and third-party clearinghouses often demands custom development or middleware, each carrying license or service fees.
2. Per-Transaction Charges: Some vendors apply fees based on claim volume, adjudication events or payment reconciliation. High-volume practices may find that these per-transaction costs eclipse flat-rate subscription models over time.
3. Support and Maintenance: Vendor support tiers vary widely. Basic packages may only cover ticket-based email support, while 24/7 phone assistance, dedicated account managers and on-site troubleshooting incur premium rates.
4. Training and Onboarding: Effective adoption requires more than user manuals. Interactive training sessions, certification programs and super-user workshops ensure staff proficiency but add to upfront and recurring costs.
Strategies to Mitigate Hidden Costs
Proactive planning and disciplined negotiation can significantly reduce unexpected expenditures. Healthcare executives should consider the following tactics:
Conduct a Total Cost of Ownership (TCO) Analysis: Map all anticipated costs over a five-year horizon, including software upgrades, support renewals and integration expenses. Quantifying each element ensures you can compare vendor proposals on an apples-to-apples basis.
Negotiate Bundled Services: Rather than licensing modules à la carte, seek package deals that incorporate essential features such as denial management, analytics and payer connectivity. Vendors are often willing to discount bundled offerings to secure larger contracts.
Cap Transaction Fees: Establish a maximum per-claim or per-transaction fee in the contract or opt for flat-rate pricing above a certain volume threshold. This approach safeguards against volume-driven cost spikes during patient surges or coding backlogs.
Audit Implementation Proposals: Scrutinize every line item in implementation quotes. Question custom development hours, third-party middleware fees and data migration estimates. Wherever possible, request fixed-fee arrangements for clearly defined deliverables.
Implementing Transparency Measures
Transparency in vendor relationships is non-negotiable. Practices can drive clarity by adopting these measures:
Regular Cost Reviews: Schedule quarterly or semi-annual reviews to reconcile actual expenditures against budgeted TCO figures. These checkpoints highlight deviations early, enabling course corrections or renegotiations.
Benchmarking: Compare your expense profile with peer institutions or industry benchmarks. Data from professional associations or regional consortia can reveal whether your costs align with market norms or if you’re paying a premium.
Performance-Based Contracts: Tie a portion of vendor compensation to key performance indicators (KPIs) such as claim submission accuracy, denial resolution time and clean claim rates. This shifts some financial risk back to the vendor and incentivizes optimal system configuration.
Leveraging Vendor Partnerships
Transform the vendor relationship from transactional to strategic. Top-performing practices collaborate closely with their software partners to unlock continuous value:
Joint Roadmapping: Participate in co-development sessions where your team and the vendor align on feature enhancements, workflow optimizations and reporting requirements. Early involvement can eliminate costly customization down the line.
Shared ROI Models: Agree on a benefit-sharing framework wherein cost savings—such as reduced denials or shorter accounts receivable cycles—are partially reinvested in ongoing support and training. This creates a virtuous cycle of improvement.
User Advisory Boards: Advocate for or join vendor-sponsored user groups. Providing feedback on functionality gaps and usability concerns ensures future releases address the real-world challenges your practice faces.
Actionable Takeaways
Hidden costs in medical billing software can undermine the very efficiency gains and revenue enhancements practices seek. By conducting a rigorous TCO analysis, negotiating transparent contracts and embracing performance-based partnerships, healthcare leaders can navigate the complexity of vendor fees and safeguard their revenue cycle. Which areas of your current software arrangement warrant a closer look? Are your contract terms aligned with your strategic financial goals? Initiating a targeted cost audit this quarter could be the first step toward a more predictable and profitable billing infrastructure.