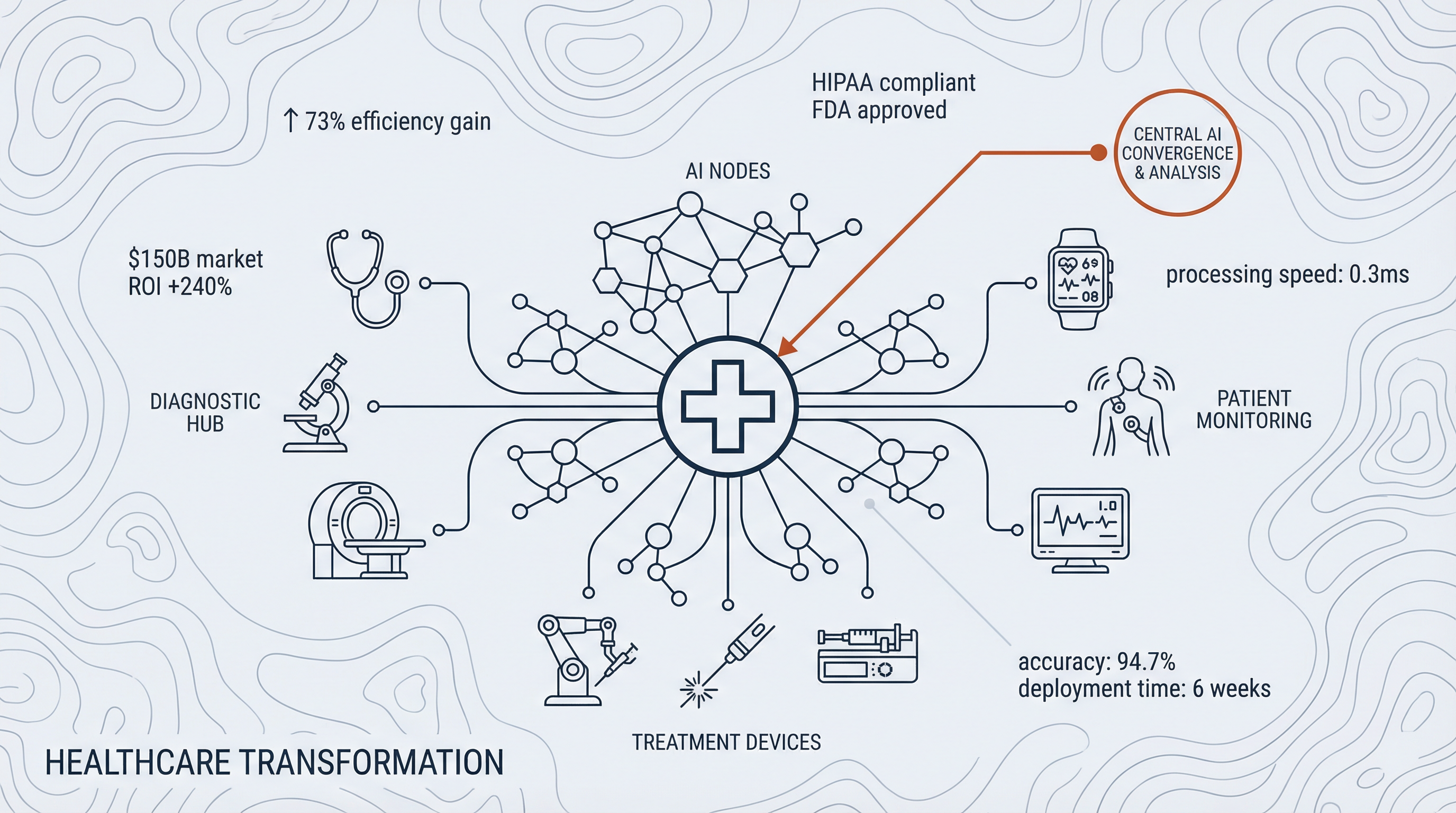
The healthcare industry is undergoing a paradigm shift driven by the rapid integration of artificial intelligence (AI) into clinical and administrative workflows. According to recent insights, adoption of AI in healthcare is significantly increasing, with two in three physicians now using some form of health AI—a 78% rise from 2023. Healthcare organizations are investing billions in AI initiatives to enhance patient care, streamline operations, and reduce costs. In this article, we explore the drivers behind this trend, the implications for patients and providers, the operational efficiencies unlocked by AI, the challenges that remain, and the future outlook for AI in healthcare.
Rising Adoption of AI by Physicians
Healthcare professionals are embracing AI tools at an unprecedented pace. As highlighted in Fierce Healthcare’s report, Why 95% of AI projects fail and how to be 5% succeed, a staggering two in three physicians now leverage some form of health AI in their daily practice. This rapid uptake reflects growing confidence in AI’s ability to support clinical decision-making, diagnostic accuracy, and treatment planning. In 2024 alone, healthcare organizations worldwide poured billions of dollars into AI initiatives, signaling a commitment to modernize care delivery models.
Key drivers of physician AI adoption include: the need for real-time data analysis, demand for personalized treatment recommendations, and pressure to improve outcomes in value-based care settings. By integrating AI tools into electronic health records (EHRs), imaging systems, and telehealth platforms, clinicians can access predictive analytics, automate routine tasks, and identify patterns that may be imperceptible to the human eye.
Implications for Patient Care
The adoption of AI is reshaping the patient experience, offering more accurate, timely, and personalized interventions. AI-driven diagnostic algorithms can analyze medical images—such as X-rays, MRIs, and CT scans—with speed and precision comparable to expert radiologists. This accelerates diagnosis for conditions like cancer, cardiovascular disease, and neurological disorders, enabling earlier interventions and improved prognoses.
Beyond diagnostics, AI supports personalized medicine by processing genomic data, patient history, and lifestyle factors to recommend tailored treatment plans. For example, predictive models can forecast patient responses to specific medications, helping physicians select therapies that maximize efficacy and minimize adverse effects. AI-powered virtual assistants and chatbots also enhance patient engagement, providing 24/7 guidance on symptom management, medication adherence, and appointment scheduling.
Patient outcomes benefit when AI augments clinical workflows. Faster diagnoses reduce the window for disease progression, while personalized treatment reduces trial-and-error approaches. As more physicians integrate AI tools, the potential for healthier, more informed patient populations grows, aligning with the broader goal of improving quality of care.
Operational Efficiency and Cost Savings
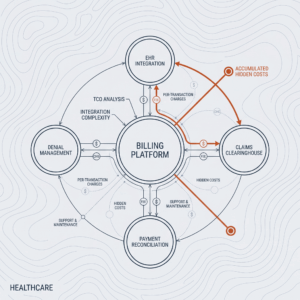
Healthcare systems face mounting pressure to control costs while maintaining high-quality care. AI offers a solution by streamlining administrative processes, reducing manual workloads, and optimizing resource allocation. Natural language processing (NLP) can automate clinical documentation, coding, and billing, freeing staff from time-consuming tasks and mitigating errors associated with manual entry.
AI-driven analytics platforms monitor patient flow, predict admission volumes, and optimize staffing schedules. By forecasting peaks in emergency department visits or inpatient census, hospital administrators can allocate beds and personnel more effectively, minimizing wait times and overcrowding. Supply chain management benefits from AI forecasting models that predict inventory needs, reducing waste from expired medications and overstocked supplies.
Financial impact is substantial: by automating repetitive tasks and improving operational workflows, healthcare organizations can reallocate human resources to direct patient care and strategic initiatives. The billions invested in AI initiatives are justified by reductions in administrative overhead, decreased readmission rates, and improved bed utilization.
Challenges and Considerations
Despite the promise of AI in healthcare, challenges persist that may hinder successful implementation. Fierce Healthcare’s analysis underscores that many AI projects struggle to move beyond pilot phases, with only a fraction achieving sustainable integration. Key barriers include data silos, lack of interoperability between systems, and concerns over data privacy and security.
Ethical considerations also play a critical role. AI algorithms trained on historical data may inadvertently perpetuate existing biases, leading to unequal care across different patient populations. Rigorous validation, transparent model development, and ongoing monitoring are essential to ensure fairness and accountability. Regulatory frameworks must evolve to oversee AI applications, guiding developers and providers toward safe, effective, and compliant solutions.
Another significant challenge is user trust. Clinicians may hesitate to rely on AI recommendations if the underlying decision processes are opaque. Developing explainable AI models that provide rationale for their outputs can bridge this trust gap, fostering collaboration between human expertise and machine intelligence.
Future Outlook for AI in Healthcare
Investment trends signal continued growth in AI adoption across a wide range of healthcare workflows. From predictive analytics for population health management to AI-powered robotics in surgery, emerging technologies promise to transform care delivery at every level. Integration of AI with the Internet of Medical Things (IoMT) will enable continuous monitoring of patient vitals, early detection of complications, and proactive interventions outside traditional care settings.
Collaborations between healthcare providers, technology vendors, and regulatory bodies will be crucial in building robust AI ecosystems. Standardized data exchange protocols, shared best practices, and multi-stakeholder governance models will drive scalable implementations. As AI matures, focus will shift from proof-of-concept projects to enterprise-wide deployments that deliver measurable clinical and financial returns.
The road ahead involves balancing innovation with caution—ensuring that AI enhances human expertise rather than replacing it. By addressing challenges related to data quality, interoperability, ethical AI design, and clinician engagement, healthcare organizations can unlock the full potential of AI to improve patient outcomes and operational efficiency.
The adoption of AI in healthcare is accelerating, and will continue to, with substantial investments and growing physician engagement. As AI tools become more sophisticated and integrated, the industry stands poised to deliver more precise, personalized, and efficient care. The journey toward widespread AI implementation will require collaboration, transparency, and a steadfast commitment to patient-centric innovations.