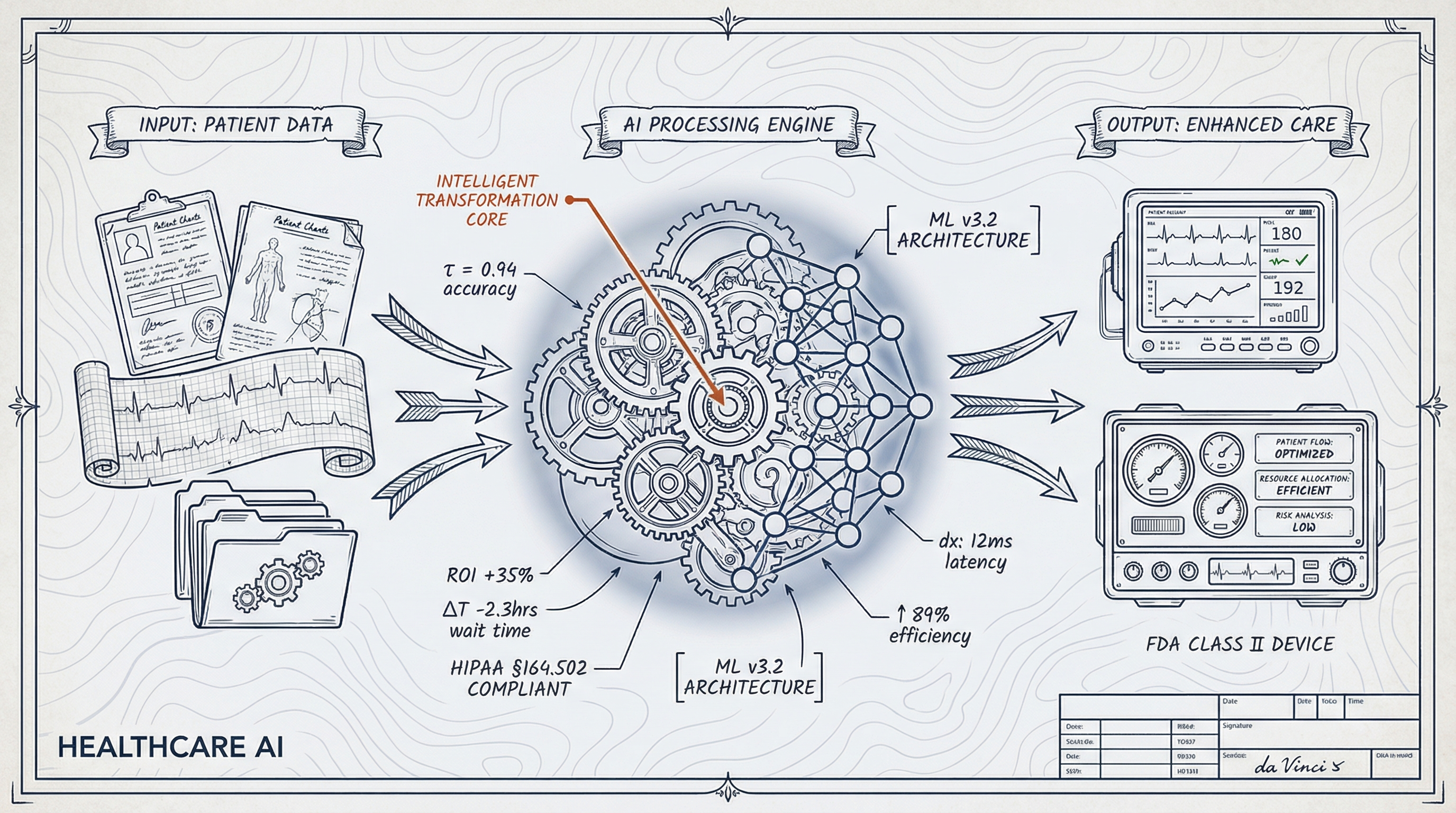
The Current State of AI Adoption in Healthcare
The adoption of AI in healthcare has grown rapidly over the past year. According to Fierce Healthcare, “Two in three physicians now use some form of health AI, up 78% from 2023, with healthcare organizations investing billions in AI initiatives.” This surge reflects a broader effort to integrate cutting-edge technologies into clinical workflows, from diagnostic support to administrative automation. Physicians are increasingly relying on AI-driven tools to analyze medical images, predict patient risk, and automate routine tasks, freeing up time for direct patient interaction.
Driving Forces Behind AI Investments
Several factors are fueling rising healthcare investment in AI initiatives:
- Technological Advances: Improvements in machine learning algorithms, natural language processing, and cloud computing have made AI solutions more accurate, scalable, and cost-effective.
- Data Availability: The proliferation of electronic health records (EHRs), wearable devices, and telemedicine platforms has generated vast amounts of structured and unstructured data for AI models to learn from.
- Economic Pressures: Healthcare systems face growing financial constraints, prompting organizations to seek AI solutions that can reduce costs, optimize staffing, and improve resource allocation.
- Regulatory Support: Agencies such as the FDA are streamlining approval processes for AI-driven medical devices and software, encouraging innovation while maintaining safety standards.
These forces converge to create an environment ripe for experimentation and large-scale deployment of AI across various healthcare domains.
Implications for Patient Care
AI-driven tools are reshaping patient care in profound ways. From diagnostics to personalized treatment plans, AI offers the potential to improve accuracy, speed, and outcomes:
- Enhanced Diagnostics: AI algorithms can analyze medical images—such as X-rays, MRIs, and CT scans—with high sensitivity and specificity. Early detection of conditions like cancer and cardiovascular disease can significantly improve prognosis.
- Predictive Analytics: Predictive models assess patient risk factors for complications, hospital readmissions, and chronic disease progression. Proactive interventions can be initiated before conditions worsen.
- Personalized Treatment: AI can sift through genetic, lifestyle, and clinical data to recommend tailored treatment plans. This approach supports precision medicine, leading to better patient adherence and reduced adverse effects.
- Virtual Health Assistants: Chatbots and virtual nurses provide 24/7 support, answering patient questions, monitoring vital signs, and scheduling appointments. This technology enhances patient engagement and satisfaction.
These applications underscore how AI is not just a tool for clinicians, but a partner in delivering more precise and empathetic care.
Operational Benefits and Efficiency Gains
Beyond clinical advantages, AI is transforming administrative and operational workflows. Healthcare organizations are leveraging AI to optimize processes, reduce waste, and allocate resources more effectively:
- Automated Documentation: Natural language processing (NLP) systems transcribe and summarize physician-patient interactions directly into EHRs, cutting down on manual entry and reducing burnout.
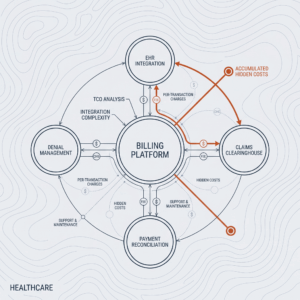
- Revenue Cycle Management: AI-driven systems detect billing errors, automate claim submissions, and predict denials, improving cash flow and reducing administrative overhead.
- Supply Chain Optimization: Predictive algorithms forecast inventory needs for medications, supplies, and equipment, minimizing stockouts and expiration-related waste.
- Staffing and Scheduling: Machine learning models analyze patient volumes, seasonal trends, and staff availability to create optimized schedules, improving patient access and reducing overtime costs.
By automating routine tasks and providing data-driven insights, AI empowers healthcare organizations to operate more smoothly and focus resources where they matter most.
Challenges and Considerations
Despite the promising benefits, the integration of AI in healthcare presents several challenges:
- Data Privacy and Security: Protecting sensitive patient data from breaches and ensuring compliance with regulations like HIPAA remains paramount.
- Integration Complexity: Incorporating AI tools into existing EHR systems and clinical workflows can be technically and logistically demanding.
- Bias and Fairness: AI models trained on non-representative datasets may produce biased outcomes, disproportionately affecting vulnerable populations.
- Physician Technology Adoption: While two in three physicians use health AI, widespread adoption requires ongoing training, change management, and trust in algorithmic recommendations.
- Regulatory and Ethical Concerns: Clear guidelines and oversight are necessary to navigate liability, informed consent, and transparency in AI-driven clinical decisions.
Addressing these challenges will require collaboration among healthcare providers, technology vendors, regulators, and patient advocacy groups to create a responsible innovation ecosystem.
Future Outlook: Rising Investment and Emerging Trends
The trend signal points to continued rising investment in AI initiatives across various healthcare workflows. Experts predict that AI will increasingly support areas such as:
- Remote Monitoring and Telehealth: Enhanced algorithms will analyze streaming patient data from wearables and home sensors, enabling real-time interventions and reducing hospital admissions.
- Genomic Medicine: AI-driven analysis of genomic data will accelerate drug discovery and facilitate truly personalized therapies.
- Robotic Surgery Assistance: AI-guided robotic systems will improve surgical precision, reduce recovery times, and expand access to minimally invasive procedures.
- Mental Health Support: Machine learning models will offer early detection of mental health conditions and deliver personalized digital therapies.
As AI capabilities expand, the role of physicians will evolve. Clinicians will act as supervisors of AI-driven processes, focusing on complex cases, ethical considerations, and human-centered care.