The data tells a clear story: 97% of employers now offer mental health coverage, and 73% report increased utilization by their workforce. This isn’t just a trend—it’s a fundamental restructuring of workplace benefits that has direct implications for healthcare practices, particularly those offering mental health services.
For small businesses, this shift represents both opportunity and challenge. Understanding the drivers behind this surge can help you position your services strategically and anticipate the needs of an expanding patient population.
The Economics Behind Employer Investment
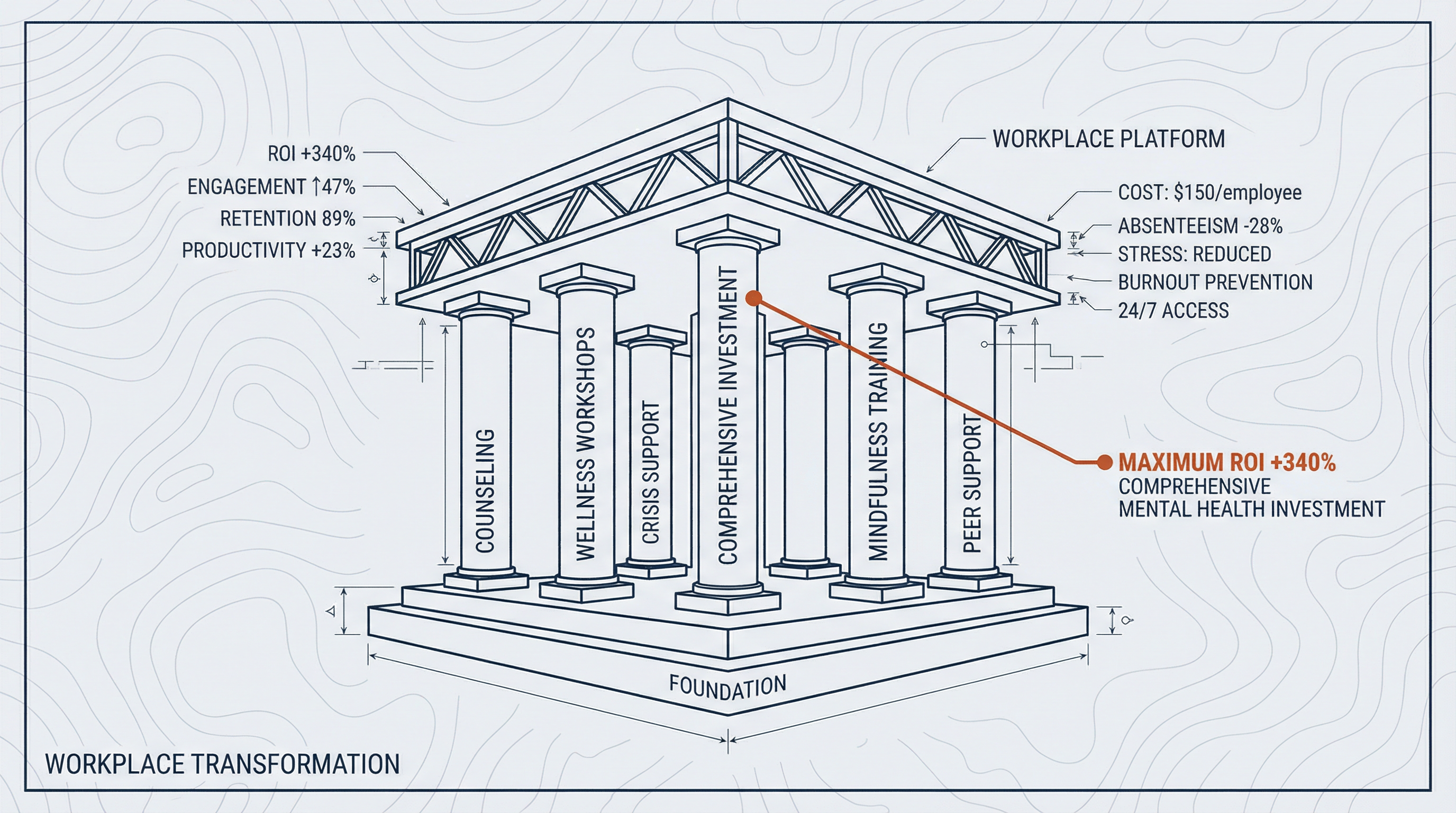
Employers aren’t expanding mental health benefits out of altruism alone. The business case is compelling: untreated mental health conditions drive absenteeism, reduce productivity, and increase turnover—all of which carry measurable costs. Organizations that invest in comprehensive mental health services report lower disability claims, higher engagement scores, and improved retention rates.
This creates a virtuous cycle. As more employees utilize mental health services, the ROI becomes clearer, which drives further investment. For your practice, this means a growing pool of insured patients with employer-sponsored coverage actively seeking mental health support.
Workforce Demographics Are Reshaping Expectations
Younger employees—particularly Millennials and Gen Z—view mental health services as non-negotiable. They expect holistic well-being support alongside traditional medical benefits, and they’re vocal about it. This generational shift is forcing employers to expand beyond basic EAP programs toward comprehensive mental health ecosystems that include teletherapy, digital tools, and specialized providers.
The delivery models are diversifying rapidly: in-person counseling, teletherapy platforms, app-based interventions, and peer support networks. For practices, this means patients increasingly expect flexible access options. The ability to offer both traditional and telehealth appointments isn’t just convenient—it’s becoming table stakes.
The Mental Health Parity Rule and Its Ripple Effects
Recent regulatory focus on mental health parity—ensuring mental health coverage matches physical health coverage—has accelerated employer action. While the rule aims to eliminate coverage disparities, it’s created compliance complexity that concerns many organizations. Administrative burdens, potential cost increases, and network adequacy requirements are real challenges employers are navigating. For businesses of every size, this regulatory landscape matters and employers need robust provider networks to demonstrate parity and value.
What High-Performing Programs Look Like
The most effective workplace mental health programs share common characteristics. They’re data-driven, using utilization metrics and employee feedback to refine offerings continuously. Leadership champions the initiatives visibly, reducing stigma from the top down. Programs integrate seamlessly with broader wellness efforts—stress management, financial counseling, resilience training—rather than operating in silos.
Communication is critical. Many programs underperform simply because employees don’t know what’s available or feel uncomfortable accessing services. Employers that succeed invest heavily in awareness campaigns and create multiple access points for care.
For businesses partnering with employers or accepting employer-sponsored insurance, understanding these program design principles helps you align your services with what organizations value most: measurable outcomes, accessibility, and employee satisfaction.
Strategic Implications for Your Practice
This surge in employer investment creates several strategic opportunities. First, consider your payer mix. Are you positioned to serve the employed, insured population that’s increasingly seeking mental health services? If you’re primarily cash-pay, is there a strategic advantage to accepting select employer-sponsored plans?
Second, evaluate your service delivery model. Can you offer the flexibility that employed patients need—evening hours, telehealth options, brief solution-focused interventions? Many employees face time constraints that make traditional 50-minute weekly sessions challenging.
Third, think about measurement. Employers increasingly expect outcomes data from their mental health investments. Practices that can demonstrate patient improvement through validated assessment tools may find themselves more attractive partners for employer-sponsored programs or direct contracting arrangements.
Navigating the Challenges
This growth isn’t without complications. Provider networks are strained, reimbursement rates often don’t reflect the true cost of quality care, and administrative requirements continue to expand. The mental health parity rule, while well-intentioned, has introduced compliance complexity that affects both employers and providers.
Cost containment remains a concern for employers, which can translate into pressure on reimbursement rates or increased utilization management. Practices need to balance accessibility with sustainability, ensuring they can serve growing demand without compromising quality or burning out clinicians.
Strategic partnerships with experienced benefit administrators and mental health-focused payers can help navigate these challenges. Value-based contracting arrangements—where reimbursement ties to outcomes rather than volume—may offer a path toward better alignment between what employers value and what practices can sustainably deliver.
The Path Forward
The shift toward comprehensive workplace mental health coverage isn’t reversing. If anything, emerging trends suggest further evolution: AI-driven assessments, personalized digital interventions, and integration of mental health data into broader well-being platforms. Employers that prioritize mental health are becoming the employers of choice for top talent.
If you are a small business, healthcare practice or wellness entrepreneur, this environment demands strategic thinking. Who is your ideal client? How does your service model align with how employed individuals access care? What outcomes can you demonstrate? These aren’t abstract questions—they’re foundational to positioning your practice in a rapidly evolving landscape.
The 97% statistic isn’t just a data point. It’s a signal that mental health services have moved from peripheral benefit to core infrastructure. Businesses that recognize this shift and adapt accordingly will find themselves well-positioned to serve a growing, increasingly diverse client population while building sustainable, resilient businesses.